One good morning, we left for an on-ground research visit to a remote village.
Everything was planned—questions, devices, roles, locations. There was a sense of excitement. Despite the off-roading and effort it took to get there, the team was energised.
When we reached, it was a very different setting. At the centre of the village was a small house. Connectivity was barely there. The setup was informal. A health worker was present, and patients were already waiting.
The sessions began, but nothing really went as planned.

Conversations were interrupted. Flows were skipped. Language became a barrier at times. Even the app stopped working due to poor network.
As the sessions progressed, things started to shift. What initially felt unstructured began to reveal patterns. We started seeing not just what we had come to find—but much more than that.
What initially felt like disruptions slowly started revealing something deeper—this was the real environment in which the product had to exist.
It led me to capture these reflections. Based on what we observed, experienced, and learned on the ground, I felt it was important to share this—so it can help product teams, designers, and founders build healthcare products with deeper empathy and realism.
Our Assumptions and The Reality
In one of the sessions, a health worker was attending to multiple patients—adults, children, and women—while using the app. She followed the flow carefully at times, but in other moments she skipped steps, paused, or moved ahead quickly. At one point, the app stopped due to connectivity. At another, she ignored a step that didn’t feel relevant in that situation.

This challenged some basic assumptions:
- We assume users behave consistently → In reality, behaviour shifts with context
- We design structured flows → Real-world flows are interrupted and non-linear
- We assume clarity on screen → Users act based on interpretation, not instruction
- We design for a defined persona → The same user operates across multiple roles
Consistency is a design goal. But in healthcare, adaptability is survival.
What Makes Healthcare UX Complex
Healthcare is not used in isolation. It lives inside dynamic, high-pressure environments.

Personas are fluid
A health worker may switch roles—caregiver, data entry operator, assistant—within the same interaction. In some cases, even patients interact with the system.
Environment is unpredictable like poor or no connectivity, crowded or constrained spaces, varying light conditions, continuous patient flow
The product is not used in ideal conditions—it is used in whatever conditions exist and behaviour is non-linear.
Users don’t always follow defined steps:
- They skip what feels unnecessary
- They take shortcuts under pressure
- They switch between tasks abruptly
In one case, a user left a flow midway to access information urgently, then returned—not where we expected, but where it made sense to them.
Designing for healthcare is not about guiding a perfect journey. It’s about supporting imperfect, real ones.
Lessons from the Ground
Users don’t behave like personas
One of the strongest realisations was that users don’t behave like personas. Personas help us think, but real behaviour is shaped by context.
The same user:
- Can be careful in one moment
- And rushed in the next
- Can follow steps in one case
- And ignore them completely in another
Design must accommodate this range—not resist it.
Environment defines UX
The environment itself plays a strong role. Connectivity may be unreliable, spaces may be crowded, lighting conditions may not be ideal, and there is often a continuous flow of patients. The product has to function within these constraints, not outside them.
Even interface decisions—like visibility, readability, speed—are deeply tied to the physical context. A system that works in a controlled demo can fail in a real setting.
Trust matters more than interface
Trust also emerged as a critical factor, often more important than the interface itself. In research, small human behaviours made a visible difference. Dressing in a way that felt familiar, sitting at the same level instead of across, and reducing any sense of hierarchy helped users open up more.
The same principle extends to the product—sudden changes can create discomfort, while familiarity builds confidence. In healthcare, trust is not an add-on; it is fundamental.
How We Conduct Research Differently
Over time, we realised that asking questions is only a small part of research. The real value comes from observing behaviour closely. What users do is often different from what they say.
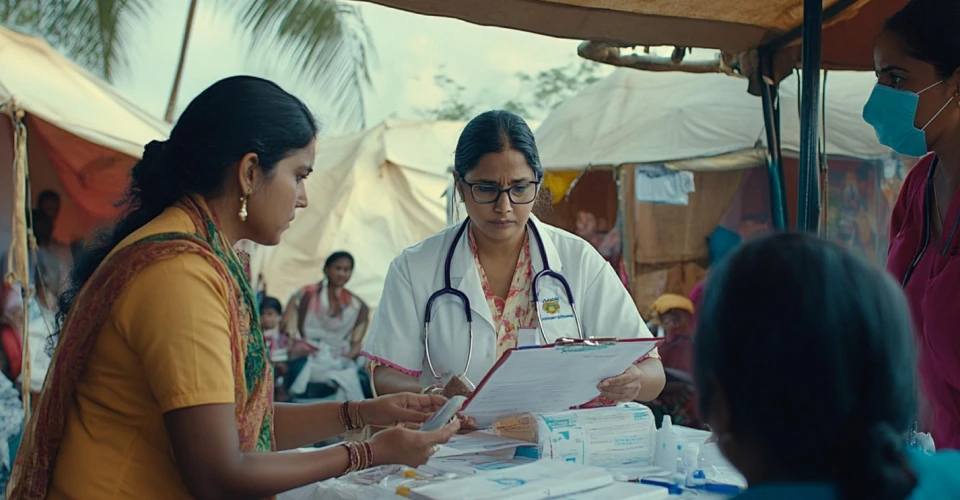
Observe actions, not just answers
We pay attention to:
- Where they hesitate
- Where they stop
- Where the flow breaks
- How they recover
These moments carry the real insight.
Let users fail comfortably
If a user struggles, we don’t intervene immediately. It’s not a test of the user, tt’s a test of the design.
We allow space for:
- Errors
- Confusion
- Self-correction
That’s where clarity emerges.
Avoid leading, stay neutral
If users look for validation, we ask:
“What do you think?”
Not to test them—but to understand their thinking.
Respect language and cultural context
Language and cultural context play a significant role as well. Understanding local vocabulary and nuances changes how insights are interpreted. Even small things—how we sit, how we speak, how we present ourselves—affect how comfortable users feel. The goal is to reduce distance and make the interaction as natural as possible.
Use structured observation techniques
- Think-aloud (gently nudged, not forced)
- Capturing physical cues
- Detailed note-taking
- Photos/recordings (with consent)
These are not processes—they are ways to see more clearly.
The Blind Spots in Most Research
Many teams rely heavily on interviews and what users say. While that is useful, it is only one part of the picture.
But what often gets missed is:
- Behaviour
- Context
- Environment
A user may say: “Yes, this is easy to use”
And still struggle when actually using it.
Design decisions based only on verbal feedback are incomplete.
Without observing reality, research becomes assumption in disguise.
What Actually Works
Effective research is less about doing more—and more about seeing & listening better.

What consistently works:
- Observation → noticing behaviour, not just outcomes
- Empathy → understanding constraints, not just tasks
- Iteration → refining based on real-world usage
Capturing micro-moments helps:
- Where users hesitate
- Where they misinterpret
- Where they abandon flows
Simple practices matter:
- Detailed notes
- Highlighting key behaviours in your notes
- Recording patterns across sessions
Closing Reflection
Designing for healthcare comes with a different kind of responsibility.
It is not just about creating efficient interfaces, but about supporting real-world care. There are constraints—privacy, compliance, and ethical boundaries—that shape what can and cannot be designed. Data visibility is not always flexible, and decisions must respect that.
More importantly, every design decision has an impact. A small confusion in interface can delay an action. A missed detail can affect someone’s experience of care.
Design, in this context, is not neutral.
It requires sensitivity, responsibility, and a deep understanding of the people it serves.































